Childhood Kidney Diseases
Frequently Asked Questions
Kidney disease can affect children in various ways, ranging from treatable disorders without long-term consequences to life-threatening conditions. Acute kidney disease develops suddenly, lasts a short time, and can be serious with long-lasting consequences or may go away completely once the underlying cause has been treated. Chronic kidney disease (CKD) does not go away with treatment and tends to get worse over time. CKD eventually leads to kidney failure, described as end-stage kidney disease or ESRD when treated with a kidney transplant or blood-filtering treatments called dialysis.
Common Kidney Diseases
The kidneys begin to develop at around 5-6 weeks gestation, and the process by which they form is complicated. If something goes wrong during development, it is possible to end up with a non-functioning kidney full of cysts and scar tissue.
Below you’ll find the most common kidney diseases in children that are presented at birth.
Polycystic Kidney Disease (PKD)
This is a condition in which many fluid-filled cysts develop in both kidneys. The cysts can multiply so much and grow so large that they lead to kidney failure. Doctors can diagnose it before or after the child is born. In some cases, there are no symptoms; in others, PKD can lead to UTIs, kidney stones, and high blood pressure. Treatment for PKD varies — some cases can be managed with dietary changes; others require a kidney transplant or dialysis.
Autosomal Recessive Polycystic Kidney Disease (ARPKD)
Autosomal recessive polycystic kidney disease (ARPKD) is a rare inherited childhood condition where the development of the kidneys and liver is abnormal. Over time, either one of these organs may fail. 1 in 20,000 people are affected by ARPKD. But in general, ARPKD is a severe condition and around 1 in 3 babies will die from severe breathing difficulties during the first 4 weeks after birth. About 8 or 9 out of 10 babies with ARPKD who survive the first month of life will live until they’re at least 5 years old.
A similar disease that emerges adults usually and that is a lot more common is called ADPKD, Autosomal Dominant Polycystic Kidney Disease. This affects 1 in 500 people and is actually a commonly seen disease among adults. ARPKD is always seen at birth.
Multicystic Dysplastic Kidney (MCDK)
(Also called kidney or renal dysplasia)
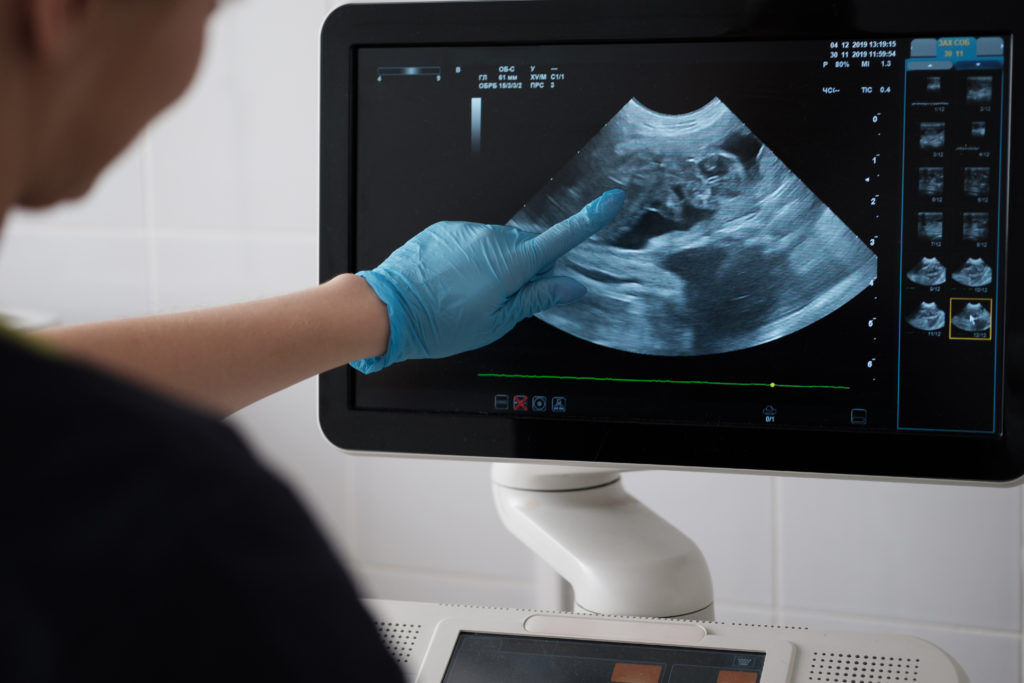
This is when large cysts develop in a kidney that hasn’t developed properly, eventually causing it to stop working. (While PKD always affects both kidneys, MCDK usually affects just one kidney.) Fortunately, the unaffected kidney takes over and most people with MCDK will have normal kidney function. MCDK usually is diagnosed by prenatal ultrasound before birth. Doctors manage it by monitoring blood pressure and screening for UTIs when needed. Very rarely, surgical removal of the kidney might be necessary.
Multicystic dysplastic kidney is thought to affect 1 in every 3,500 people, but that number may be higher because some people who have it are never diagnosed with the condition.
There are rare cases when multicystic dysplastic kidney runs in families because of a genetic trait. However, the vast majority occur as a sporadic event. The proper formation of a kidney is complex with hundreds of thousands of steps that must execute correctly. If there is a hiccup in just one step, an abnormal kidney may form. Some studies suggest certain viral infections and some drugs might also play a role if exposure occurs at a critical stage of development.
If both kidneys are affected, a miscarriage may occur. This is because the kidneys are responsible for the production of amniotic fluid which is required to maintain a normal pregnancy. Amniotic fluid is also important for proper lung development.
Babies with severe kidney dysplasia affecting both kidneys that do survive birth may need the following early in life:
- blood-filtering treatments called dialysis
- a kidney transplant
Childhood nephrotic syndrome
Childhood nephrotic syndrome is not a disease in itself; rather, it is a group of symptoms that
- indicate kidney damage—particularly damage to the glomeruli, the tiny units within the kidney where blood is filtered
- result in the release of too much protein from the body into the urine
When the kidneys are damaged, the protein albumin, normally found in the blood, will leak into the urine. Proteins are large, complex molecules that perform a number of important functions in the body.
The two types of childhood nephrotic syndrome are
- primary—the most common type of childhood nephrotic syndrome, which begins in the kidneys and affects only the kidneys
- secondary—the syndrome is caused by other diseases
A health care provider may refer a child with nephrotic syndrome to a nephrologist—a doctor who specializes in treating kidney disease. A child should see a pediatric nephrologist, who has special training to take care of kidney problems in children, if possible. However, in many parts of the country, pediatric nephrologists are in short supply, so the child may need to travel. If traveling is not possible, some nephrologists who treat adults can also treat children
Posterior Urethral Valve Obstruction
This narrowing or obstruction of the urethra affects only boys. It can be diagnosed before the baby is born or just after and is treated with surgery.
Fetal Hydronephrosis
This enlargement of one or both of the kidneys is caused by either an obstruction in the developing urinary tract or a condition called vesicoureteral reflux (VUR) in which urine abnormally flows backward (or refluxes) from the bladder into the ureters. Fetal hydronephrosis is usually diagnosed before the child is born and treatment varies widely. In some cases the condition only requires ongoing monitoring; in others, surgery must be done to clear the obstruction from the urinary tract.
Hemolytic Uremic Syndrome
Hemolytic uremic syndrome, or HUS, is a kidney condition that happens when red blood cells are destroyed and block the kidneys’ filtering system. Red blood cells contain hemoglobin—an iron-rich protein that gives blood its red color and carries oxygen from the lungs to all parts of the body.
When the kidneys and glomeruli—the tiny units within the kidneys where blood is filtered—become clogged with the damaged red blood cells, they are unable to do their jobs. If the kidneys stop functioning, a child can develop acute kidney injury—the sudden and temporary loss of kidney function. Hemolytic uremic syndrome is the most common cause of acute kidney injury in children.
Renal Tubular Acidosis (RTA)
Renal tubular acidosis (RTA) is a disease that occurs when the kidneys fail to excrete acids into the urine, which causes a person’s blood to remain too acidic. Without proper treatment, chronic acidity of the blood leads to growth restriction, kidney stones, bone disease, chronic kidney disease, and possibly total kidney failure.
